Main Line Rheumatology is more mobile! Our improved mobile website now makes it easier for you to be well informed, every day! Read all about our doctors, get office information, learn more about diseases we treat, read about us in the News, and catch up on daily social media posts ~ all in one place. Come visit!
Author Archives: Nina Greberman
Can Stem Cells Regenerate Damaged Cartilage in Osteoporosis?
If you have arthritis, you know about the term “bone on bone”. We tell patients that you cannot grow new cartilage once it is destroyed, whether from over or repetitive use, the  natural aging process, or injury. Stories about stem therapy being used to treat osteoarthritis, an aggressive degenerative form of arthritis, are popular on the internet. But, can stem cells regenerate damaged cartilage with this disease? Maybe one day we can be cautiously optimistic, but for today, I am still skeptical.
natural aging process, or injury. Stories about stem therapy being used to treat osteoarthritis, an aggressive degenerative form of arthritis, are popular on the internet. But, can stem cells regenerate damaged cartilage with this disease? Maybe one day we can be cautiously optimistic, but for today, I am still skeptical.
Our understanding is that stem cells are the building blocks of all human tissue. Arthritis, or joint degeneration, is due to loss of the cartilage that cushions bones and the stem cell goal is to treat arthritis to regrow cartilage.
Stem cells that come from your own body and are harvested through a medical scientific procedure, are then injected back into your body (stem cell therapy) in a desired location, addressing a specific medical condition, movement or pain problem. A newborn baby’s umbilical cord is rich in natural stem cells, and there has been a movement over the last 5-10 years to freeze and save these stem cells for that baby’s (or natural family member) possible health needs.
The human body is a remarkable repair machine. Skin can regenerate, and a small piece of liver transplanted in a human body, grows miraculously to accommodate the body’s needs. But damaged cartilage causing osteoarthritis, does not naturally regenerate. Making degenerated and damaged bones and joints “almost good as new” is more often than not, only the outcome of surgery.
Dr. Shane Shapiro, at the Mayo Clinic Orthopedic Surgery and Center for Regenerative Medicine, published an article in May, 2018 describing how efforts and studies in stem cell regenerative medicine could treat degenerative conditions such as osteoarthritis, changing the course of orthopedic surgery over the coming years. Although research and studies show promise, stem cell treatment for arthritis is not widely available at this time, as is still being researched.
When discussing stem cell therapy, it’s important to understand that pure stem cells are not currently available to U.S. patients outside of a clinical research study. Stem cell therapies currently used outside clinical studies do not contain pure stem cells; they are a mix of a variety of cells with only a very small percentage, stem cells.
A handful of clinical research trials, monitored by the U.S. Food and Drug Administration (FDA), are ongoing at this time to study stem cell treatment for arthritis. The early findings are encouraging for the future. Many stem cell therapies now marketed to patients are conducted without a required FDA biologics license. Also, some forms of stem cell therapies are mislabeled, and do not contain actual living stem cells. These practices cause concern among rheumatologists as these treatments may mislead, or even harm the public.
Research into stem cells and arthritis shows that there are opportunities for stem cell treatment resulting mostly in pain relief and improvement in function, or quality of life. But only a few limited early studies have demonstrated improvement in new cartilage or bone formation needed to cure arthritis, so I am skeptical. Exactly how that cartilage regrowth occurs, or even how pain relief is achieved, is still unknown.
To conclude, here is my opinion. Stem cell therapy, particularly with fetal stem cells, offers great promise for many diseases, including regenerating the damaged cartilage of osteoarthritis. Free standing stem cell clinics that offer treatment, giving you back a few of your mature stem cells for a high cost. As a cautionary tale, The New York Times reported, October 15, 2018, that Harvard University is retracting data that had implied that stem cells had improved cardiac function, when stem cells were placed in the heart. The odds of success currently are minimal, and insurance does not cover this expensive procedure. The “Religious Right” has prevailed upon the last three administrations to toss umbilical cords into the trash instead of utilizing them to save or improve lives. We hope this will change one day, or maybe other countries can lead the way.
Gary V. Gordon, MD, FACP, FACR Awarded 2018 Rheumatologist of the Year by The Arthritis Foundation
Gary V. Gordon, MD, FACP, FACR, Chief of Rheumatology, Lankenau Medical Center, Wynnewood, PA received the 2018 Rheumatologist of the Year Award from The Arthritis Foundation. He is pictured with Holly Maddams, Executive Director of the Arthritis Foundation, Eastern PA. Dr. Gordon was honored on October 5, 2018 at The Arthritis Foundation’s Bone Bash, held at Mutter Museum of The College of Physicians of Philadelphia.
pictured with Holly Maddams, Executive Director of the Arthritis Foundation, Eastern PA. Dr. Gordon was honored on October 5, 2018 at The Arthritis Foundation’s Bone Bash, held at Mutter Museum of The College of Physicians of Philadelphia.
If Gout is a Disease of the Rich, Why Do I Have It?
Gout is a disease that has literally been known to man, since antiquity.
Gout was historically known as “the disease of kings” or “rich man’s disease” especially 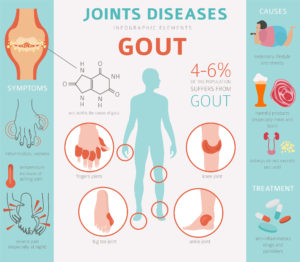 during the Depression, because it was thought to be caused by a “rich” diet, heavy in meat. The first documentation of gout was from Egypt in 2,600 BC, in a description of arthritis of the big toe.
during the Depression, because it was thought to be caused by a “rich” diet, heavy in meat. The first documentation of gout was from Egypt in 2,600 BC, in a description of arthritis of the big toe.
Gout is characterized by recurrent attacks of a red, tender, hot, and swollen joint, often the joint of a big toe. However, any joint can be involved including the spine or rare occasion. The first attack can come on rapidly, out of nowhere and normally intensifies over less than 12 hours. Patients will say that even contact with a bed sheet can be excruciating.
Who gets gout? Gout affects about 1 to 2% of the Western population at some point in their lives, and has become more common in recent decades. Medical risk factors include obesity, diabetes, hypertension, kidney failure and metabolic syndrome, which is a cluster of conditions including high blood pressure, high blood sugar, excess abdominal body fat and abnormal cholesterol or triglyceride levels that together, increase the risk of heart disease, stroke and diabetes. Diuretics, alcohol binge drinking, and certain foods (see below) are risk factors.
Sometimes you just cannot help that you have gout! It is partly genetic as family history increases your risk, and older males are most commonly affected. Gout is no longer considered the “rich man’s disease” as it has no socioeconomic factor.
Approximately 50% of gout cases are due to persistently elevated levels of uric acid the blood. Simply explained, uric acid is a chemical produced when your body breaks down foods that contain organic compounds called purines. Foods and beverages with a high purine content include liver and other organ meats, anchovies, mackerel, dried beans and other legumes, spinach, dried mushrooms, seaweed, high-fructose drinks, beer and wine. Uric acid is eliminated in our urine, but some people cannot eliminate as well as others. When too much uric acid remains in the blood, it can form sharp crystals which deposit in the joints, tissues and tendons, resulting in a “gouty attack”. The more frequently this happens, the more joints tend to be involved with each attack.
A rheumatologist is the best doctor to diagnose and treat gout, since gout is a form of inflammatory arthritis, and rheumatologists are arthritis war czars! It is important to drain fluid from a joint, examine it under a special microscope and establish the diagnosis. This is especially important for short and long term treatment as other medical problems (i.e. joint infections) can look similar. Your rheumatologist will examine, diagnose and treat your gout, while making lifestyle and diet recommendations so you experience fewer attacks.
How does gout present itself, and how do you know when to see a rheumatologist? Gout signs or symptoms present in multiple ways, although the most usual is a recurrent attack of acute inflammatory arthritis with a red, tender, swollen joint that feels hot. The joint at the base of the big toe is affected most often, accounting for 50% of the cases we see, and other joints – heels, knees, wrists, and fingers, may also be affected. Joint pain usually begins over a few hours during the night while sleeping, mainly due to lower body temperature. Sometimes other symptoms may occur along with the joint pain including fatigue, a high fever, or tophi (singular-tophus) which are hard, painless deposits of uric acid crystals in joints, cartilage and bones or other places on the body. Tophi can look very scary to the observer, but are treatable,
Gout treatment is divided into two parts: acute attack medication and prevention. Medication such as non-steroidal anti-inflammatory drugs (NSAIDS) or cortisone will alleviate pain and provide improvement within twenty-four hours. Without treatment, an acute attack of gout usually resolves in five to seven days, however, 60% of people have a second attack within one year. Those with gout are at increased risk of high blood pressure, diabetes, metabolic syndrome, and kidney and cardiovascular disease-thus increased risk of death.
Your gout is treatable and with medical care, lifestyle and diet changes can be controlled. See your rheumatologist and get with a program!
Why are my Prescription Bills so Ridiculously High?
 Drug costs continue to rise and Americans continue to feel the pain in their wallets.
Drug costs continue to rise and Americans continue to feel the pain in their wallets.
A nationally representative Consumer Reports survey of almost 1,200 adults who currently take a prescription drug, found that high costs are forcing people to cut back on housing or groceries, stay in jobs longer-delaying retirement, stay in jobs they cannot stand, or take on a second job. People can feel so desperate that they sometimes make potentially dangerous choices, such as rationing or stop taking the medication for periods of time.
As prescribing physicians, we know that Americans spend more on drugs than people in any other country. As a rheumatologist, I know that many diseases and ailments can only be treated with certain medications, so patients get better and have an appropriate quality of life. We stay informed with breaking news and drug cost statistics while make every attempt to prescribe medication conscientiously, keeping in mind purpose. But as doctors and not drug sales reps, or pharmacies, we frequently don’t know drug costs. Our practice learned that back in 2016, total drug costs went up 6.3% compared with the year before, about three times the rate for other goods and services, according to the Department of Labor. According to this report, out-of-pocket drug costs are still rising; from $25 billion in 2000 to a projected $67 billion in 2025!
The bad news is that nothing stops drug companies from charging the highest prices that the market will bear. According to AARP, (https://www.aarp.org/health/drugs-supplements/info-2017/rx-prescription-drug-pricing.html) prescription drug prices in America are among the highest in the world. Why do other countries (like Canada) negotiate better with drug companies, and the U.S. allows drug companies to set their own prices? The US government allows “government-protected monopolies” for certain drugs, preventing generics from coming to market to reduce prices. Sometimes, state laws and other “well-intentioned” federal policies limit generics’ abilities to keep costs down. The FDA takes a long time to approve generic drugs, and studies show that there are often three to four year waits before generic manufacturers can win approval to make drugs not protected by patents
A drug manufacturer holds patent rights on a new drug. That gives the manufacturer a monopoly on the drug for the 20-year life of the patent. During that time, the manufacturer can raise the price as frequently and as much as the market will bear. It’s about supply and demand. When the demand for a drug is high, drug companies raise prices. When it’s a new drug with plenty of advertising dollars behind it, and consumers see TV commercials promising a cure, drug companies charge premium prices.
Here are some factors that also drive up drug costs:
Patent law. Pharmaceutical companies strategize how to extend their monopoly on a drug beyond the expiration of its original patent, seeking approval for a “new” product that is a slight variation on the original. The longer that a drug company maintains its monopoly, the longer it can continue to charge whatever it wants.
Limits on Medicare. One of the largest purchasers of prescription drugs, Medicare is blocked by law from negotiating prices. When Congress was debating the law that created Medicare Part D (which took effect in 2006), lobbyists from the pharmaceutical industry convinced legislators that giving Medicare negotiating power would amount to price control.
Multiple middlemen. When you pick up a drug at the pharmacy, you don’t know its real price; that is established between the manufacturer and your insurer. You just pay the agreed-upon copay rate.
There is nothing illegal with any of this: publicly owned corporations, pharmaceutical firms focus on their bottom line and do whatever they want.
How can you “shop” drug prices? We know that if we need a new stove, we shop around and pick the best model at the price we can afford. This creates competition that keeps pricing competitive. Not so with prescription drugs! Doctors and health care providers don’t always have pricing for various drugs available, so they themselves cannot comparison shop. Most doctors write prescriptions for the drugs they know work well, and believe it or not, the Food and Drug Administration (FDA) doesn’t require drug companies to prove that their new products are better than existing products.
There is some good news. Twenty-Four States Passed 37 Bills to Curb Rising Rx Drug Costs in the Short 2018 Legislative Session. https://nashp.org/twenty-states-passed-37-bills-to-curb-rising-rx-drug-costs-in-the-short-2018-legislative-session/
The bottom line, is consumers need help with their prescription drug costs TODAY. An educated consumer can ask their doctor, “What does this drug cost?” and then comparison shop until the US government takes responsibility. A rheumatologist can hope.
Oh My Aching Back!
As rheumatologists, how many times a week do you think we see patients in our office, and the first words we hear are, “Oh, my aching back!” or “My back went out, and I have  no idea what I did.” A LOT!
no idea what I did.” A LOT!
Optimally, we should be able to comfortably stand up straight and walk down the street; right? We expect to have a spine supported by our muscles and tendons, so our back is strong and we can walk, go up and down steps, get in and out of a car, bed or the bathtub, as well as do work around the house, move and lift items, etc.
But sometimes that is just not meant to be, and here’s why.
Unfortunately, millions of Americans have ongoing back pain. There are often issues with spinal joints, discs, muscles, or nerves working together during movement, causing pain. The problem can arise from natural aging, injury or disease.
Depending on the underlying cause of back pain, symptoms can be experienced in a variety of ways. You may have:
- Pain that worsens after prolonged sitting or standing
- Dull pain in the lower back
- Stinging or burning pain in the lower back moving to the backs of the thighs, lower legs or feet
- Numbness or tingling (sciatica)
- Tightness in the lower back, pelvis or hip muscle spasms making it difficult to stand up straight, walk, or go from standing to sitting
- Your doctor will ask you to describe your pain. Here is how we categorize pain symptoms:
In addition, symptoms of lower back pain are usually described by type of onset, location and duration:
- Acute back pain typically comes on suddenly. Lasting for a few days or weeks, it is considered a normal response to injury or tissue damage. Pain gradually subsides as the body heals.
- Sub-acute low back pain is more prolonged, lasting between 6 weeks-3 months, and is usually due to muscle strain or joint pain.
- Chronic back pain is more severe, lower back pain that lasts over 3 months, and might not respond to initial treatments.
- Regional (localized) back pain or referred pain which radiates down one or both legs below the knees.
The most important goal is to address your back pain with your rheumatologist during an examination to determine if any of these issues are your problem:
Disease: Arthritis is a common cause of back pain.
Herniated or slipped discs: Discs are between your spine’s vertebrae and are “shock absorbers”. Lower back or hip pain associated is usually caused by wear and tear, or age.
Degenerative disc disease: Pain can be age-related, where discs shrink or tear, causing the bones to rub together.
Inflammation of the sacroiliac joint: Located where the spine and pelvis come together, swelling and eroding joint cartilage can occur from injury, arthritis, an infection, or pregnancy.
Spinal stenosis: Affecting those over age 60, pressure on the spine and nerves can cause the legs and shoulders to feel numb, burning and weak.
Pinched Nerve: Usually caused by a bone spur, or a herniated disc. Sciatica with pain down the back of a leg into the foot is a typical example.
Spondylolisthesis: Degenerative form of arthritis which weakens the joints and ligaments that keep the spine aligned.
Accidents and Injuries: Automobile, falls, muscle sprains or fractures.
Spine or vertebral fractures: Occurring from a fall, injury or osteoporosis.
Sprains and strains: Injuries to muscles, tendons and ligaments that support the spine and joints.
Spasms: Sometimes when muscles and tendons are torn in the lower back.
Lifestyle: Back pain can come from lifting, being overweight, lack of exercise, slouching and even smoking.
Emotions: Stress can cause muscle tension in the back, and depression and anxiety may make pain feel worse.
What can help alleviate back pain? Medications, stretching exercises and weight loss are helpful. Other medical experts such as physiatrists, osteopaths and orthopedic surgeons may also be necessary to try and resolve back issues.
Your rheumatologist’s goal is to alleviate your back pain so you feel better, move more comfortably, and live the healthy and active life you are meant to enjoy!
Why Am I Height Challenged?
 Everybody wants to maintain optimal height during their adult lifetime. But height loss is a common part of the aging process. We may notice tall elderly people with great posture, but unfortunately, they are a distinct minority.
Everybody wants to maintain optimal height during their adult lifetime. But height loss is a common part of the aging process. We may notice tall elderly people with great posture, but unfortunately, they are a distinct minority.
There are two kinds of height loss. All of sudden at a doctor’s office visit, you find out you are an inch shorter. Commonly heard is “I used to be 5’8 and now I’m 5’6; what happened?” The other height loss is more noticeable, being bent over. We don’t like that any better, but we’re more aware of that physical change which may be accompanied by pain or discomfort.
As we age, height loss often occurs as the soft discs, which sit between the vertebral bones in our backs lose water and don’t do their job, maintaining your previous height. This type of height loss is subtle and painless. More acute height loss is often accompanied by significant pain in the mid-back region, corresponding to the thoracic spine, resulting from a compression fracture or collapse of one of the bony vertebrae. We see a lot of this as a consequence to osteoporosis (a silent disease defined by a decrease in bone mass resulting in an increased risk of fracture). The most important piece of information you can seek is an evaluation as to why you have osteoporosis.
An x-ray or a DEXA bone density study is valuable to provide information about osteopenia (you might be in the beginning stage of possible height loss) fractures and/or osteoporosis, all of which can compromise height. The DEXA, which can include a lateral picture of the thoracic spine, will make the diagnosis of a compression fracture. If the fracture occurs without severe trauma such as a car accident or fall off a ladder, it is considered a fragility or low-impact fracture; an example is a fall from a standing position to the floor. Even if the DEXA results are normal, patients still need treatment for osteoporosis. Men need to be evaluated for causes of osteoporosis such as steroid exposure (i.e. prednisone) or low testosterone. More rare causes need evaluation for such problems as multiple myeloma, a form of cancer.
Sometimes, kyphoplasty, where a radiologist places “medical cement” into the collapsed vertebra, can prevent further height loss and stabilize the spine. It is vitally important to do everything possible to treat osteoporosis and vertebral compression fractures. Like dominoes, the first compression fracture is the greatest risk for the next one, so treatment and stabilization should be undertaken as soon as possible.
In addition to medical evaluation and tests, as with everything we do to maintain good health and a quality of life, here is what our bones and spine health deserve and benefit from: a nutritious and balanced diet, exercise and fresh air, and proper rest. Our bodies are fantastic machines that can benefit from proper maintenance!
Is Dr. Google Smarter Than My Doctor?
Most patients who are curious and comfortable using the internet, often go to Google to check out information that their doctor gave them during an office visit. Is Dr. Google always dependable or useful? Sometimes.
While online, patients visit websites, enter chat rooms or interact online with friends and family in the differential diagnosis of possibilities that might prove helpful in finding additional information, helping to facilitate a full and accurate diagnosis and treatment plan. On the other hand, not all websites, chat rooms or friends and family’s opinions are created equal. I have found the most dependable information on medical school-related websites such as Harvard, Johns Hopkins, Mayo Clinic, U Penn and Stanford University. In comparison and in my medical opinion, I often disagree with information presented on WebMD and Drugs.com, among other websites.
It is helpful in maintaining a good and trusted relationship with your doctor to ask whether information you have discovered makes sense in your medical condition, or case. Confronting your doctor and saying he or she is “wrong” and that you have discovered “correct” data from WebMD, for example, not only weakens your doctor-patient trust bond, but can burn bridges and end up being of little help. Today, patients want to be informed consumers. I applaud being curious and responsible in the quest for answers; this is our new normal. But some medical information available to patients online, even on trusted websites as above, can be easily misunderstood or read out of context, such as listed medication side effects, or even dangerous drug combinations. Every patient is an individual. Every medical condition is unique to each individual patient. Let your doctor who is your trusted medical partner and knows your personal medical history, listen to everything you have to share and about your concerns and address your diagnosis and treatment.
When watching TV drug commercials, if you are a patient with a certain condition or disease, you know the frightened reaction you may have when hearing about serious drug side effects, especially the biologics which doctors use to treat rheumatoid and psoriatic arthritis. Are they real side effects that could actually affect you? Yes and no. The drug manufacturer is concerned about liability and being sued for not stating a list of potential side effects, and after seeing the commercial, we ask ourselves, “Why would anyone in their right mind take on such risk?” For example, most of these commercials talk about cancer and lymphoma. To the best of my knowledge, there are no recent studies showing an increase in the frequency of solid tumors. Lymphomas occur more commonly in rheumatoid arthritis, regardless of whether patients are on a biologic (drug) agent, and it is still unclear whether the biologic drugs like Humira or Enbrel, increase the risk of lymphomas. Not treating an active disease like rheumatoid or psoriatic arthritis, can have its own obvious consequences.
So what is the conclusion? An ounce of prevention is worth a pound of cure. Be an informed consumer, discuss with your doctor and together, agree on the right treatment for you.


